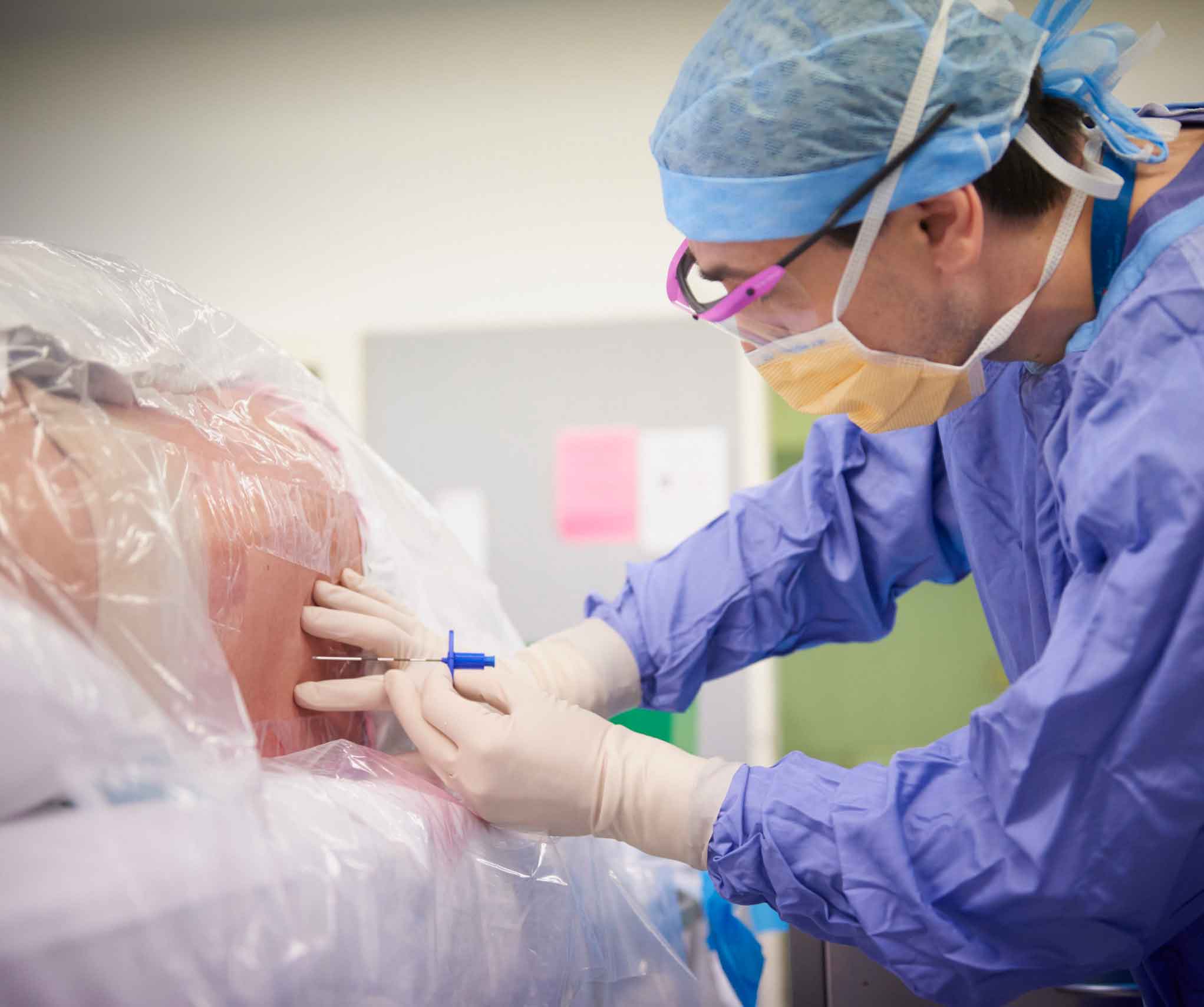
What is an epidural steroid injection (ESI)?
Epidural steroid injection (ESI) is a minimally invasive procedure used to help manage pain associated with various conditions that affect the spinal cord, including spinal disc disease, nerve impingement, spinal canal stenosis, and shingles. ESI involves the injection of local anesthetic and a steroid into the epidural space, which is the fat-filled space that surrounds the outer layers of the spinal cord.
In the spinal canal the epidural is a fat filled space that surrounds the outer layers of the spinal cord from the base of your skull to the tailbone. It contains important structures including blood vessels, spinal nerves and lymphatic vessels. The fat filled space acts as a shock absorber to protect these important structures.
The epidural space can be injected with local anaesthetic (numbing agent) and steroid to help relieve the pain associated with a number of conditions, including:
- Spinal disc disease including disc herniation
- Nerve impingement such as ‘sciatica’
- Spinal canal stenosis (narrowing of the spinal canal)
- Shingles and post herpetic neuralgia
- Pain associated with the labour and delivery of pregnancy
What are the different types of ESI?
There are different types of ESI’s based on the approach that is taken to access the epidural space. The use of these approaches are determined on a case by case basis and will have been discussed with you prior to your procedure. These include:
Interlaminar: needle is inserted between the bones in your spine.
Caudally directed: needle and catheter is inserted at an opening between the lowest end of your spine and tailbone.
Transforaminal: needle is inserted at an opening in the side of your spine where the nerves leave the spinal cord.
How effective is an ESI?
The effectiveness of an ESI does depend on the condition being treated and does vary from patient to patient. It is difficult to predict your outcome before the procedure. In general, patients can see reductions in pain for up to 6 months. In some rarer cases it can go up to 1 year and can allow any nerve compression to get better and not return. If there is at least 3-6 months of relief than ESI’s can be safely repeated.
It is important to recognise that an ESI is not a cure for your condition(s). In some cases it can help give the injured area time to heal. In general however it should be looked upon as a symptomatic treatment that can then be used to facilitate reduction in medication and improve quality of life and functioning. Any improvement to pain seen can be used to facilitate a rehabilitation approach to your management as guided by your treating doctor.
How is an ESI done?
An ESI is a minimally invasive procedure completed in a clean operating theatre environment. It is usually completed as a day procedure and usually does not take more than 10 minutes. Throughout the entire procedure your heart rate, blood pressure and oxygen levels will be monitored. In addition to your doctor there will be an anaesthetist who will monitor your care during the procedure.What to expect
- You will be given a sedative through a drip to relax you so that you are not aware of the procedure (this is not a general anaesthetic).
- The procedure is completed under x-ray guidance to help direct the needle involved in the injection.
- The procedure will involve injecting a special dye to confirm the correct location of the injection.
- The area to be targeted will be cleansed with an antiseptic solution. A local anaesthetic will then be injected in the treatment area before the epidural needle is inserted to help numb the skin.
- A small amount of anaesthetic and steroid is then injected into the epidural space.
Are there any risks with an ESI?
The risks of complications with ESI’s are low. There are risks associated with the procedure, medications used and the anaesthesia. For risks relating to the anaesthesia we recommend discussing this with your anaesthetist.
Potential risks include:
Common (usually mild and self-limiting)
- Bleeding at the injection site
- Bruising and discomfort at the site of injection
- Limb weakness
- Difficulty passing urine
- Ineffective
Uncommon
- Steroid effects: elevated blood sugar levels, sleep disturbance, mood changes, facial flushing, sweating
- Headaches
- Nausea and/or vomiting
- Worsening of your pain
Rare
- Nerve or spinal cord damage
- Infection
- Bleeding causing spinal cord compression
- Allergic reaction to medications
Is an ESI right for you?
If you think an ESI may be right for you talk to your doctor about it. If you would like any further information or would like to see one of our doctors please do not hesitate to contact Anodyne.